Most hair transplant discussions revolve around visible factors: graft count, technique names, devices, or before-and-after photos.
However, the true success or failure of a hair transplant is decided at a level patients never see — the microvascular network of the scalp.
Microvascular damage is rarely mentioned in marketing materials, yet it remains one of the leading hidden causes of poor growth, low density, and disappointing long-term results.
As a surgeon, I consider microvascular preservation not an advanced concept, but a foundational requirement of ethical hair transplant surgery.
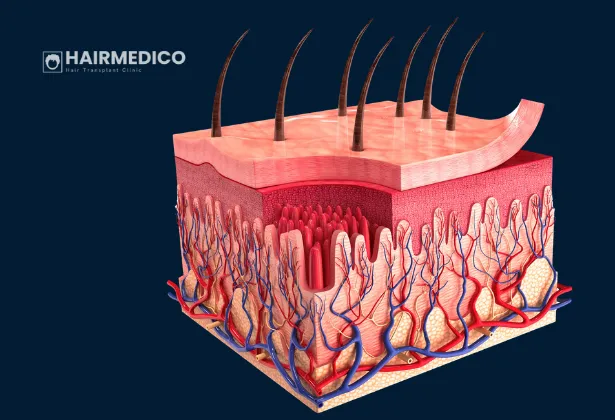
Microvasculature refers to the smallest blood vessels in the scalp:
Capillaries
Arterioles
Venules
Each transplanted follicular unit survives only if:
Oxygen delivery is sufficient
Nutrient diffusion remains intact
Waste removal is uninterrupted
Hair follicles are metabolically active mini-organs. Without an intact microvascular environment, even perfectly extracted grafts cannot survive.
Microvascular injury is almost never caused by a single mistake.
It is the result of cumulative surgical stress, often linked to high-volume or poorly planned procedures.
Common causes include:
Excessive incision density in a limited area
Aggressive or deep recipient site creation
Prolonged surgery duration without tissue rest
Repeated trauma to the same vascular zones
Inadequate spacing between grafts
Each of these factors alone may appear insignificant. Combined, they can severely compromise blood flow.
One of the most dangerous misconceptions is equating absence of necrosis with vascular safety.
Microvascular damage is often:
Subclinical
Invisible to the naked eye
Only evident months later
Patients may experience:
Patchy or uneven regrowth
Delayed growth beyond expected timelines
Poor crown density despite high graft numbers
By the time these signs appear, the vascular damage has already done its work.
The crown (vertex) has:
Naturally lower vascular density
Spiral hair orientation requiring complex incision angles
Higher metabolic demand for cosmetic density
This makes it particularly sensitive to microvascular overload.
Attempting to implant high graft density in the crown without respecting vascular limits is one of the most common causes of disappointing outcomes.
This is why Hairmedico approaches crown restoration conservatively and strategically, as part of a holistic hair transplant plan.
👉 Learn more about our surgical philosophy here: https://hairmedico.com/hair-transplant
Large single-session graft numbers increase:
Tissue edema
Interstitial pressure
Capillary compression
When capillaries are compressed, oxygen diffusion drops.
Even if blood flow technically exists, functional ischemia develops.
This explains why some high-graft surgeries show:
Early shedding without regrowth
Thin, weak hair shafts
Inconsistent density patterns
The issue is not extraction quality — it is recipient bed viability.
Microvascular safety cannot be standardized by protocols alone.
It requires continuous intraoperative judgment, including:
Adjusting incision depth dynamically
Modifying density based on bleeding response
Allowing tissue recovery periods during surgery
Respecting patient-specific scalp characteristics
These decisions cannot be automated, delegated, or rushed.
This is one of the core reasons Hairmedico operates under a surgeon-led, single-patient-per-day model.
In high-volume clinics, speed is often prioritized over physiology.
This leads to:
Uniform density patterns applied to all patients
Ignored scalp variability
Technician-driven implantation without vascular feedback
Hair transplant surgery becomes a production process — not a medical one.
True microvascular preservation requires slowing down, observing tissue response, and adapting in real time.
Microvascular damage does not only affect immediate growth.
Long-term risks include:
Reduced scalp elasticity
Increased fibrosis
Compromised future transplant options
Accelerated miniaturization in surrounding native hair
In revision cases, surgeons often face irreversible vascular compromise, limiting corrective possibilities.
At Hairmedico, microvascular integrity guides every surgical decision:
Controlled incision density
Adaptive graft distribution
Staged implantation strategy
Conservative crown planning
Surgeon-performed critical steps
Our pricing reflects the procedure itself — not graft volume promises.
👉 You can review our transparent surgical approach here: https://hairmedico.com/price
Microvascular health is not an optional detail.
It is the biological foundation of hair transplant success.
Patients deserve to understand that:
More grafts do not equal better results
Blood supply sets the real limit
Surgical restraint is a sign of expertise, not limitation
A successful hair transplant respects the scalp as a living system — not a canvas to be filled.
If you are considering a hair transplant, ask your clinic how they protect microvascular circulation, not just how many grafts they plan to implant.
A properly planned surgery today prevents irreversible disappointment tomorrow.
Bu cevap Dr. Arslan Musbeh tarafından onaylanmıştır.
Your consultant is ready to answer your hair transplant questions, and you can also get a personalized online hair analysis.